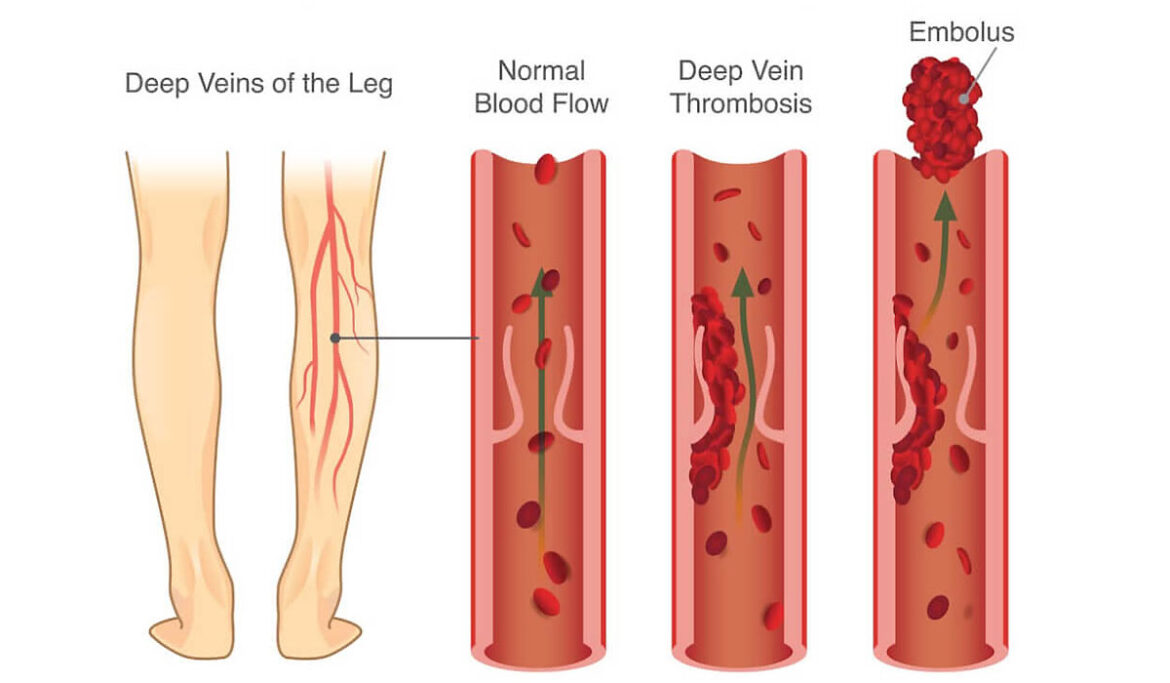
Deep Vein Thrombosis (DVT) occurs when a blood clot (thrombus) forms in one or more of the deep veins in your body, usually in legs. DVT can cause leg pain or swelling, but may occur without any symptoms.
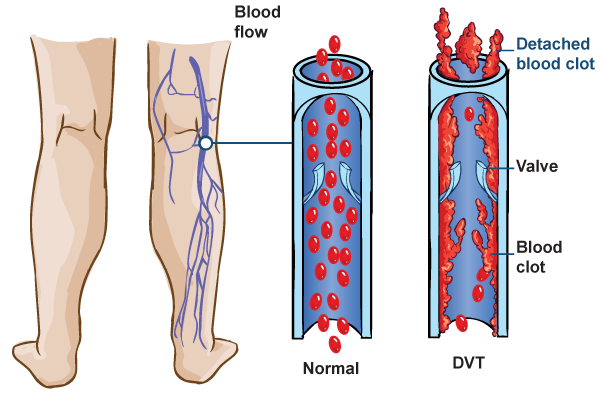
It is a life-threatening condition because blood clots in your veins can break loose, travel through your bloodstream and lodge in your lungs, blocking blood flow. Pulmonary embolism may result in loss of life.
DVT is curable with medicines and other treatments. It can also be prevented with few changes in lifestyle.
Symptoms of Deep Vein Thrombosis (DVT)
Deep Vein Thrombosis (DVT) may or may not have visible symptoms. Some common signs are:
- Swelling in foot, ankle, or leg, usually on one side or in very rare cases both the legs.
- Pain in your leg. Often the pain starts in your calf. It feels like cramping or a soreness.
- Severe, unexplained pain in your foot and ankle.
- An area of skin that feels warmer than the skin on the surrounding areas.
- Skin over the affected area turning pale or a reddish or bluish color.
Causes of Deep Vein Thrombosis (DVT)
DVT occurs most commonly in people who are over 50 years in age. Certain conditions that alter how your blood moves through your veins can raise your risk of developing clots. These include:
- Having an injury that damages your veins.
- Carrying extra weight, especially around your middle, puts more pressure on the veins in your pelvis and legs, which can double your risk of DVT. If your body mass index (BMI) is 25 or more and you are also taking hormonal birth control pills, the risk is as much as tenfold.
- Having a family history of DVT.
- Having a catheter placed in a vein.
- Taking birth control pills or undergoing hormone therapy.
- Smoking may cause DVT. Any amount of smoking, even just occasionally, damages your heart and blood vessels. Be extra careful not to smoke if you also take birth control pills. The combination could result in almost nine times the normal risk for DVT.
- Premature Birth is a surprising cause behind DVT. Though there are no concrete proofs, scientists have deduced that DVT is mostly seen in people who had a premature birth.
- Staying seated for a long time while you are at your desk at hob, in a car or on a plane.
- Hereditary blood clotting disorders.
- Cancer can cause tissue damage and release chemicals that trigger clotting. Cancers have the highest rates of DVT. Clots are a common side effect of lymphomas, leukemia, and liver cancer. Some types of chemotherapy also make clots more likely.
- Heart failure, a condition that makes it more difficult for your heart to pump blood.
- Surgery has a major risk of DVT. Surgeries on the lower extremities, such as joint replacement surgery.
- Being pregnant increases your risk of DVT. Increased hormone levels, and a slower blood flow as your uterus expands and restricts blood flowing back from your lower extremities, contribute to this risk. This elevated risk continues until about six weeks after giving birth. Being on bed rest or having a C-section also increases your risk of having DVT.
Diagnosing Deep Vein Thrombosis (DVT)
Diagnosing Deep Vein Thrombosis requires certain specific tests. In many cases there are hardly any symptoms so you need
D-dimer test
A specialized blood test called a D-dimer test is effective to diagnose DVT. This test detects pieces of blood clot that have been broken down and are loose in your bloodstream. The larger the number of fragments found, the more likely it is that you have a blood clot in your vein. Though sometimes the finding are not very clear and are inconclusive.
Ultrasound scan
An ultrasound scan can be used to detect clots in your veins. A special type of ultrasound called a Doppler ultrasound can also be used to find out how fast the blood is flowing through a blood vessel. This helps identify when blood flow is slowed or blocked, which could be caused by a blood clot.
Venogram
A venogram may be used if the results of a D-dimer test and ultrasound scan cannot confirm a diagnosis of DVT.
During a venogram, a liquid called a contrast dye is injected into a vein in your foot. The dye travels up the leg and can be detected by X-ray, which will highlight a gap in the blood vessel where a clot is stopping the flow of blood.
Treatment of Deep Vein Thrombosis (DVT)
DVT treatments focus on keeping the clot from growing. In addition, treatment attempt to prevent a pulmonary embolism and lower your risk of having more clots.
Medication
Your doctor may prescribe medications that thin your blood, such as heparin and warfarin. This drugs makes it harder for your blood to clot. It also keeps existing clots as small as possible and also decreases chance to get more clots.
If blood thinners don’t work or if you have a severe case, thrombolytic drugs administered intravenously work by breaking up clots.
Compression Stockings
Wearing compression stockings can lower your chance of developing clots. On daily use it helps in the proper function of the veins without getting new clots. The stockings reach just below your knee or a little above it. Swelling in your feet are also under control.
Inferior Vena Cana Filters
You might need to have a filter put inside the large abdominal vein called the vena cava if you are not able to consume blood thinners. This form of treatments helps prevent pulmonary embolisms by stopping clots from entering your lungs.
Complications of Deep Vein Thrombosis (DVT)
The two main complications of deep vein thrombosis (DVT) are pulmonary embolism and post-thrombotic syndrome.
Pulmonary embolism
A pulmonary embolism is the most serious complication of DVT. It happens when a piece of blood clot (DVT) breaks off and travels through your bloodstream to your lungs, where it blocks one of the blood vessels. In severe cases this can be fatal.
If the clot is small, it might not cause any symptoms. If it is medium-sized, it can cause breathing difficulties and chest pain. A large clot can cause the lungs to collapse and result in heart failure and also death. About 1 in 10 people with an untreated DVT develops a severe pulmonary embolism.
Post-thrombotic syndrome
If you have had a DVT, there are chances to develop long-term symptoms in your calf known as post-thrombotic syndrome. This affects around 20-40% of people with a history of DVT.
If you have DVT, the blood clot in the vein of your calf can divert the flow of blood to other veins, causing an increase in pressure. This can affect the tissues of your calf and lead to symptoms like calf pain, swelling, a rash and ulcers on the calf (in severe cases).
DVT in the thigh vein, increases the risk of post-thrombotic syndrome occurring. It is also more likely to occur if you are overweight or if you have had more than one DVT in the same leg.
Prevention of Deep Vein Thrombosis (DVT)
To prevent deep vein thrombosis, some common preventive measures include the following:
- Take any prescribed medications as directed. If you are having surgery, you will be given blood thinners especially if the operation of lower limbs. Your doctor may also prescribe aspirin or other medications that help prevent clots to be taken for a while after surgery.
- Avoid sitting still. If you have had surgery or have been on bed rest for other reasons, try to get moving as soon as possible. If you are sitting for a while, try not to cross your legs because this can limit blood flow. If you’re traveling a long distance by car, stop every hour or so and walk around.
- If you are on a plane, try to stand or walk occasionally. If you can’t do that, at least try to exercise your lower legs. Try raising and lowering your heels while keeping your toes on the floor, then raising your toes while your heels are on the floor. Stretch your legs with simple movements.
- Make lifestyle changes. Lose weight and quit smoking. Extra weight and the unhealthy habit of smoking is a deadly combination for DVT.
- Get regular exercise. Exercise lowers your risk of blood clots, which is especially important for people who have to sit a lot or travel frequently.
[ You may also read on Orthopedics Surgery in India ]
Related posts:
Importance of Rehab after Knee and Hip Replacement Surgery
Tips to Prevent Fractures in Osteoporosis